Breast editorial
With the new ultra-sensitive, high resolution digital infrared cameras available today, a technology that has been developing over the past 20 years is creating renewed interest. Canadian researchers recently found that infrared imaging of breast cancers could detect minute temperature variations related to blood flow and demonstrate abnormal patterns associated with the progression of tumors. These images or thermograms of the breast were positive for 83% of breast cancers compared to 61% for clinical breast examination alone and 84% for mammography.
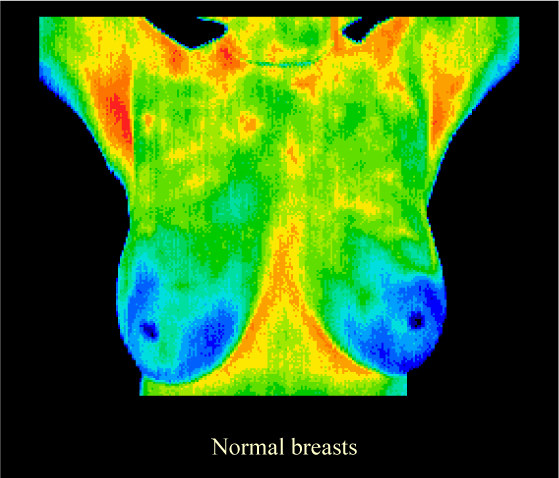
Thermography, as a physiologic test, demonstrates heat patterns that are strongly indicative of breast abnormality. The test can detect subtle changes in breast temperature that indicate a variety of breast diseases and abnormalities; and once abnormal heat patterns are detected in the breast, follow-up procedures including mammography are necessary to rule out or properly diagnose cancer and a host of other breast diseases such as fibrocystic syndrome, Pagets disease, etc.
By performing thermography years before conventional mammography, a selected patient population at risk can be monitored more carefully, and then more accurately utilize mammography or ultrasound as soon as is possible to detect the actual lesion – (once it has grown large enough and dense enough to be seen on mammographic film). This can increase the patients treatment options and ultimately improve the outcome.
It is in this role that thermography provides its most practical benefit to the general public and to the medical profession. It is certainly an adjunct to the appropriate usage of mammography and not a competitor. In fact, thermography has the ability to identify patients at the highest risk and actually increase the effective usage of mammographic imaging procedures.
Until such time as a cure has been found for this terrible disease, progress must be made in the fields of early detection and risk evaluation coupled with sound clinical decision making.
Thermography, with its non-radiation, non-contact and low-cost basis has been clearly demonstrated to be a valuable and safe early risk marker of breast pathology, and an excellent case management tool for the ongoing monitoring and treatment of breast disease when used under carefully controlled clinical protocols.